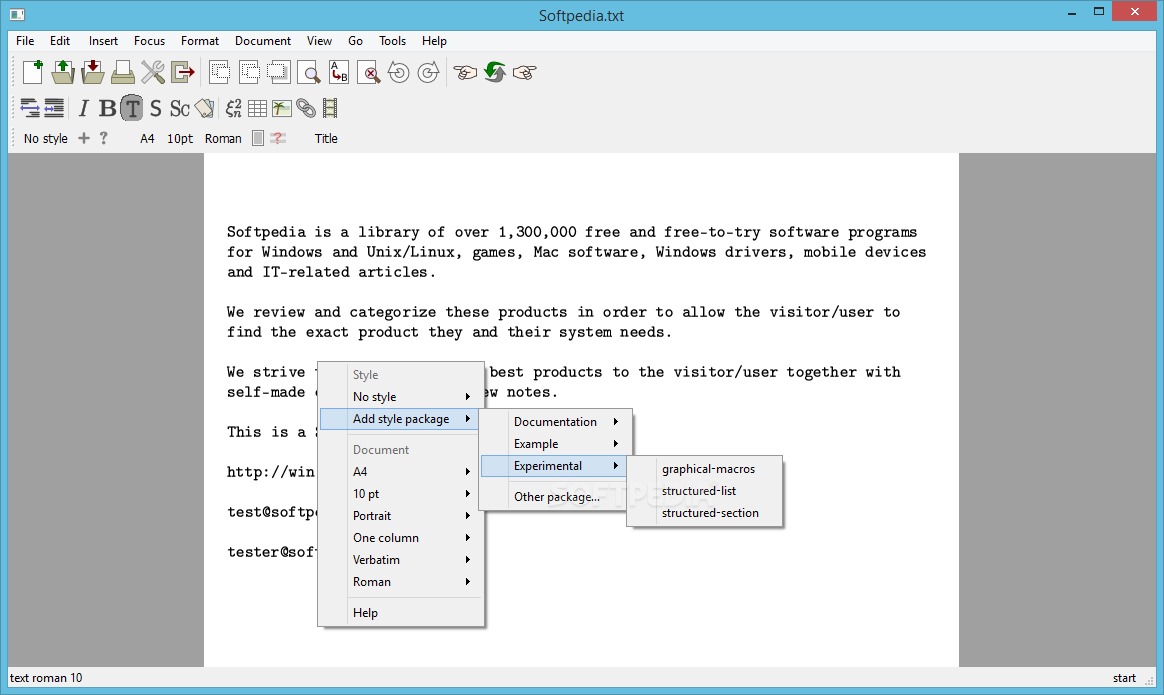
Here, we used fluorescent imaging microscopy and ex vivo assays to compare the activation and distribution of CAR T cells upon contact with malignant B cells and carcinoma cells. Whether similar molecules and mechanisms control the antitumoral action of CAR T cells remain to be established. When T cells are stimulated by a variety of external stimuli, including antigens and chemokines, the affinity and clustering of LFA-1 increases in an inside-out signaling process that promotes the binding of this integrin to ICAM-1 ( 9).  
LFA-1 is an integrin expressed by T cells and other hematopoietic cells and binds to intercellular adhesion molecule 1 (ICAM-1) expressed by antigen-presenting cells, as well as by some tumor cells. The importance of chemokines and their receptors in attracting CAR T cells and promoting their contact with malignant cells has also been recognized and therapeutically exploited in mouse tumor models ( 6).Īmong adhesion molecules, two integrins, lymphocyte function-associated antigen-1 (LFA-1) and CD103 (αE/β7), play a critical role in T cell–tumor cell interactions ( 7, 8). Much attention has been paid to the expression of the target antigen, and decreased expression of the targeted molecule at the surface of tumor cells has been recognized as a major cause of CAR T-cell resistance ( 5). Up to now, little is known about the elements that promote CAR T-cell interactions with their targets. After overcoming these stromal obstacles, T cells need to infiltrate tumor islets to carry out cytotoxic activity. As a result, interactions between T cells and tumor cells are impaired. 4) hinder antitumor functions of T cells in progressing lung tumors by reducing their migration and sequestering them in the stroma. 2, 3) and tumor-associated macrophages (TAM ref. Using an experimental system of human tumor slices combined with dynamic imaging microscopy, we previously demonstrated that a dense extracellular matrix (ECM refs. Once within the tumor, T cells must expand, persist, and mediate cytotoxicity in a hostile environment largely composed of immunosuppressive cells and molecules. In carcinomas, lymphocytes have to navigate through a dense stroma that surrounds cancer cells. This could be due, at least in part, to the existence of various physical and environmental barriers in solid tumors, which are less present in hematologic cancers. The requirement for IFNγ and ICAM-1 to enable CAR T-cell entry into tumor islets is of significance for improving CAR T-cell therapy in solid tumors.Īdoptive immunotherapy with gene-engineered chimeric antigen receptor (CAR) T cells has demonstrated efficacy in several B-cell malignancies but not yet in solid tumors ( 1). The ICAM-1/LFA-1 interaction interference, through antibody or shRNA blockade, prevented CAR T-cell enrichment in tumor islets. The analysis of this two-step entry process showed that activated CAR T cells triggered the upregulation of ICAM-1 on tumor cells in an IFNγ-dependent pathway. After this initial peripheral activation, EGFR CAR T cells progressively relocated to the center of tumor cell regions. By comparison, EGFR CAR T cells only initially interacted with a subset of carcinoma cells located at the periphery of tumor islets. Our results indicated that CD20 CAR T cells rapidly form productive ICAM-1–dependent conjugates with their targets. Here, we used fluorescent imaging microscopy and ex vivo assays to compare the early functional responses (migration, Ca 2+, and cytotoxicity) of CD20 and EGFR CAR T cells upon contact with malignant B cells and carcinoma cells. Adoptive transfer of T cells expressing chimeric antigen receptors (CAR) has shown remarkable clinical efficacy against advanced B-cell malignancies but not yet against solid tumors.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
